Related Research Articles

Menopause, also known as the climacteric, is the time when menstrual periods permanently stop, marking the end of reproduction. It typically occurs between the ages of 45 and 55, although the exact timing can vary. Menopause is usually a natural change. It can occur earlier in those who smoke tobacco. Other causes include surgery that removes both ovaries or some types of chemotherapy. At the physiological level, menopause happens because of a decrease in the ovaries' production of the hormones estrogen and progesterone. While typically not needed, a diagnosis of menopause can be confirmed by measuring hormone levels in the blood or urine. Menopause is the opposite of menarche, the time when a girl's periods start.

A progestogen, also referred to as a progestagen, gestagen, or gestogen, is a type of medication which produces effects similar to those of the natural female sex hormone progesterone in the body. A progestin is a synthetic progestogen. Progestogens are used most commonly in hormonal birth control and menopausal hormone therapy. They can also be used in the treatment of gynecological conditions, to support fertility and pregnancy, to lower sex hormone levels for various purposes, and for other indications. Progestogens are used alone or in combination with estrogens. They are available in a wide variety of formulations and for use by many different routes of administration. Examples of progestogens include natural or bioidentical progesterone as well as progestins such as medroxyprogesterone acetate and norethisterone.

Estrone (E1), also spelled oestrone, is a steroid, a weak estrogen, and a minor female sex hormone. It is one of three major endogenous estrogens, the others being estradiol and estriol. Estrone, as well as the other estrogens, are synthesized from cholesterol and secreted mainly from the gonads, though they can also be formed from adrenal androgens in adipose tissue. Relative to estradiol, both estrone and estriol have far weaker activity as estrogens. Estrone can be converted into estradiol, and serves mainly as a precursor or metabolic intermediate of estradiol. It is both a precursor and metabolite of estradiol.
Bioidentical hormone replacement therapy (BHRT), also known as bioidentical hormone therapy (BHT) or natural hormone therapy, is the use of hormones that are identical on a molecular level with endogenous hormones in hormone replacement therapy. It may also be combined with blood and saliva testing of hormone levels, and the use of pharmacy compounding to obtain hormones in an effort to reach a targeted level of hormones in the body. A number of claims by some proponents of BHT have not been confirmed through scientific testing. Specific hormones used in BHT include estrone, estradiol, progesterone, testosterone, dehydroepiandrosterone (DHEA), and estriol.

Estradiol acetate (EA), sold under the brand names Femtrace, Femring, and Menoring, is an estrogen medication which is used in hormone therapy for the treatment of menopausal symptoms in women. It is taken by mouth once daily or given as a vaginal ring once every three months.

Drospirenone is a progestin and antiandrogen medication which is used in birth control pills to prevent pregnancy and in menopausal hormone therapy, among other uses. It is available both alone under the brand name Slynd and in combination with an estrogen under the brand name Yasmin among others. The medication is an analog of the drug spironolactone. Drospirenone is taken by mouth.
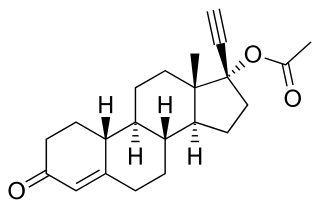
Norethisterone acetate (NETA), also known as norethindrone acetate and sold under the brand name Primolut-Nor among others, is a progestin medication which is used in birth control pills, menopausal hormone therapy, and for the treatment of gynecological disorders. The medication available in low-dose and high-dose formulations and is used alone or in combination with an estrogen. It is ingested orally.

An estrogen patch, or oestrogen patch, is a transdermal delivery system for estrogens such as estradiol and ethinylestradiol which can be used in menopausal hormone therapy, feminizing hormone therapy for transgender women, hormonal birth control, and other uses. Transdermal preparations of estrogen are metabolized differently than oral preparations. Transdermal estrogens avoid the first pass through the liver and thus potentially reduce the risk of blood clotting and stroke.
Hypoestrogenism, or estrogen deficiency, refers to a lower than normal level of estrogen. It is an umbrella term used to describe estrogen deficiency in various conditions. Estrogen deficiency is also associated with an increased risk of cardiovascular disease, and has been linked to diseases like urinary tract infections and osteoporosis.
Hormone replacement therapy (HRT), also known as menopausal hormone therapy or postmenopausal hormone therapy, is a form of hormone therapy used to treat symptoms associated with female menopause. Effects of menopause can include symptoms such as hot flashes, accelerated skin aging, vaginal dryness, decreased muscle mass, and complications such as osteoporosis, sexual dysfunction, and vaginal atrophy. They are mostly caused by low levels of female sex hormones that occur during menopause.
Menerba, also known as Menopause Formula 101 (MF-101), is a botanical drug candidate that acts as a selective estrogen receptor modulator (SERM) which is being studied for its potential to relieve hot flashes associated with menopause. Menerba, an estrogen receptor beta (ERβ) agonist (ERBA), is part of a new class of receptor subtype-selective estrogens, which is selective in transcriptional regulation to one of the two known estrogen receptor (ER) subtypes. Menerba consists of 22 herbs that have been used historically in traditional Chinese medicine.
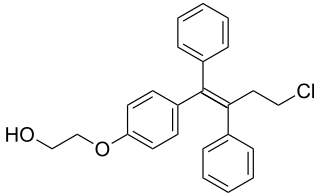
Ospemifene is an oral medication indicated for the treatment of dyspareunia – pain during sexual intercourse – encountered by some women, more often in those who are post-menopausal. Ospemifene is a selective estrogen receptor modulator (SERM) acting similarly to an estrogen on the vaginal epithelium, building vaginal wall thickness which in turn reduces the pain associated with dyspareunia. Dyspareunia is most commonly caused by "vulvar and vaginal atrophy."

Conjugated estrogens (CEs), or conjugated equine estrogens (CEEs), sold under the brand name Premarin among others, is an estrogen medication which is used in menopausal hormone therapy and for various other indications. It is a mixture of the sodium salts of estrogen conjugates found in horses, such as estrone sulfate and equilin sulfate. CEEs are available in the form of both natural preparations manufactured from the urine of pregnant mares and fully synthetic replications of the natural preparations. They are formulated both alone and in combination with progestins such as medroxyprogesterone acetate. CEEs are usually taken by mouth, but can also be given by application to the skin or vagina as a cream or by injection into a blood vessel or muscle.

Estradiol (E2) is a medication and naturally occurring steroid hormone. It is an estrogen and is used mainly in menopausal hormone therapy and to treat low sex hormone levels in women. It is also used in hormonal birth control for women, in feminizing hormone therapy for transgender women, and in the treatment of hormone-sensitive cancers like prostate cancer in men and breast cancer in women, among other uses. Estradiol can be taken by mouth, held and dissolved under the tongue, as a gel or patch that is applied to the skin, in through the vagina, by injection into muscle or fat, or through the use of an implant that is placed into fat, among other routes.

Progesterone (P4), sold under the brand name Prometrium among others, is a medication and naturally occurring steroid hormone. It is a progestogen and is used in combination with estrogens mainly in hormone therapy for menopausal symptoms and low sex hormone levels in women. It is also used in women to support pregnancy and fertility and to treat gynecological disorders. Progesterone can be taken by mouth, vaginally, and by injection into muscle or fat, among other routes. A progesterone vaginal ring and progesterone intrauterine device used for birth control also exist in some areas of the world.

Fezolinetant, sold under the brand name Veozah among others, is a medication used for the treatment of hot flashes (vasomotor symptoms) due to menopause. It is a small-molecule, orally active, selective neurokinin-3 (NK3) receptor antagonist which is under development by for the treatment of sex hormone-related disorders. It is taken by mouth. It is developed by Astellas Pharma which acquired it from Ogeda (formerly Euroscreen) in April 2017.

An estrogen (E) is a type of medication which is used most commonly in hormonal birth control and menopausal hormone therapy, and as part of feminizing hormone therapy for transgender women. They can also be used in the treatment of hormone-sensitive cancers like breast cancer and prostate cancer and for various other indications. Estrogens are used alone or in combination with progestogens. They are available in a wide variety of formulations and for use by many different routes of administration. Examples of estrogens include bioidentical estradiol, natural conjugated estrogens, synthetic steroidal estrogens like ethinylestradiol, and synthetic nonsteroidal estrogens like diethylstilbestrol. Estrogens are one of three types of sex hormone agonists, the others being androgens/anabolic steroids like testosterone and progestogens like progesterone.

Estetrol (E4) is an estrogen medication and naturally occurring steroid hormone which is used in combination with a progestin in combined birth control pills and is under development for various other indications. These investigational uses include menopausal hormone therapy to treat symptoms such as vaginal atrophy, hot flashes, and bone loss and the treatment of breast cancer and prostate cancer. It is taken by mouth.

The pharmacology of estradiol, an estrogen medication and naturally occurring steroid hormone, concerns its pharmacodynamics, pharmacokinetics, and various routes of administration.
References
- ↑ "Hot Flashes - Symptoms and causes - Mayo Clinic". www.mayoclinic.org. Retrieved 31 March 2021.
- ↑ University of Glasgow (24 October 2007). "Doctors seek the key to understanding hot flushes". University News (Archive of news). University of Glasgow. Retrieved 19 April 2013.
- ↑ "Menopause". About.com. n.d. Archived from the original on 9 March 2011. Retrieved 19 April 2013.
- ↑ Bunyavanich S (6 June 2007). "Low Testosterone Could Kill You". ABC News. ABC News Internet Ventures. Retrieved 20 April 2013.
- ↑ "Hot Flashes in Men: An Update". Harvard Medical School. March 2014. Retrieved 5 May 2020.
- ↑ Petering, Ryan C.; Brooks, Nathan A. (1 October 2017). "Testosterone Therapy: Review of Clinical Applications". American Family Physician. 96 (7): 441–449. ISSN 0002-838X. PMID 29094914.
- ↑ "What to Expect During Therapy". Lupron Depot. Abbott Laboratories. Retrieved 20 April 2013.
- ↑ "Hot Flashes in Men -- Mayo Clinic Researchers Describe A Treatment". ScienceDaily. Science Daily LLC. 19 October 2004. Retrieved 20 April 2013.
- ↑ Engstrom CA, Kasper CE (March 2007). "Physiology and endocrinology of hot flashes in prostate cancer". American Journal of Men's Health. 1 (1): 8–17. doi: 10.1177/1557988306294162 . PMID 19482779. S2CID 20123822.
- ↑ Anitei S (16 April 2007). "Men Can Experience Hot Flashes, Just Like Women in Menopause". Softpedia. Retrieved 20 April 2013.
- ↑ Utian WH (1 June 2012). "Recent Developments in Pharmacotherapy for Vasomotor Symptoms". Current Obstetrics and Gynecology Reports. 1 (2): 43–49. doi: 10.1007/s13669-012-0009-4 . ISSN 2161-3303.
- ↑ Shanafelt TD, Barton DL, Adjei AA, Loprinzi CL (November 2002). "Pathophysiology and treatment of hot flashes". Mayo Clinic Proceedings. 77 (11): 1207–18. doi:10.4065/77.11.1207. PMID 12440557.
- 1 2 Freedman RR (July 2014). "Menopausal hot flashes: mechanisms, endocrinology, treatment". The Journal of Steroid Biochemistry and Molecular Biology. Current Views of Hormone Therapy for Management and Treatment of Postmenopausal Women. 142: 115–20. doi:10.1016/j.jsbmb.2013.08.010. PMC 4612529 . PMID 24012626.
- ↑ Spetz AC, Zetterlund EL, Varenhorst E, Hammar M (November–December 2003). "Incidence and management of hot flashes in prostate cancer". The Journal of Supportive Oncology. 1 (4): 263–6, 269–70, 272–3, discussion 267-8, 271–2. PMID 15334868.
- ↑ Moustakli E, Tsonis O (29 November 2023). "Exploring Hormone Therapy Effects on Reproduction and Health in Transgender Individuals". Medicina. 59 (12): 2094. doi: 10.3390/medicina59122094 . PMC 10744413 . PMID 38138197.
- ↑ Magon N (October–December 2011). "Gonadotropin releasing hormone agonists: Expanding vistas". Indian Journal of Endocrinology and Metabolism. 15 (2): 261–267. doi: 10.4103/2230-8210.85575 . PMC 3193774 . PMID 22028996.
- ↑ Casimiro I (13 February 2019). "Severe Vasomotor Symptoms Post-Oophorectomy Despite Testosterone Therapy in a Transgender Man: A Unique Case Study". Journal of the Endocrine Society. 3 (4): 743–736. doi:10.1210/js.2018-00367. PMC 6436763 . PMID 30931422.
- ↑ Mueller A, Haeberle L, Zollver H, Claassen T, Kronawitter D, Oppelt PG, Cupisti S, Beckmann MW, Dittrich R (1 September 2010). "Effects of Intramuscular Testosterone Undecanoate on Body Composition and Bone Mineral Density in Female-to-Male Transsexuals". The Journal of Sexual Medicine. 7 (9): 3190–3198. doi:10.1111/j.1743-6109.2010.01912.x. PMID 20584125.
- ↑ U.S. Food and Drug Administration (10 February 2004). "FDA Updates Hormone Therapy Information for Post Menopausal Women". FDA News Release (Archived content). U.S. Food and Drug Administration. Retrieved 19 April 2013.
- ↑ Rossouw JE, Anderson GL, Prentice RL, LaCroix AZ, Kooperberg C, Stefanick ML, et al. (July 2002). "Risks and benefits of estrogen plus progestin in healthy postmenopausal women: principal results From the Women's Health Initiative randomized controlled trial". JAMA. 288 (3): 321–33. doi: 10.1001/jama.288.3.321 . PMID 12117397.
- ↑ Serock MR, Wells AK, Khalil RA (November 2008). "Modulators of vascular sex hormone receptors and their effects in estrogen-deficiency states associated with menopause". Recent Patents on Cardiovascular Drug Discovery. 3 (3): 165–86. doi:10.2174/157489008786263970. PMID 18991792.
- ↑ Løkkegaard E, Andreasen AH, Jacobsen RK, Nielsen LH, Agger C, Lidegaard Ø (November 2008). "Hormone therapy and risk of myocardial infarction: a national register study". European Heart Journal. 29 (21): 2660–8. doi: 10.1093/eurheartj/ehn408 . PMID 18826989.
- ↑ "For Women - Menopause and Hormones: Common Questions". Food and Drug Administration .
- ↑ Santen RJ, Allred DC, Ardoin SP, Archer DF, Boyd N, Braunstein GD, et al. (July 2010). "Postmenopausal hormone therapy: an Endocrine Society scientific statement". The Journal of Clinical Endocrinology and Metabolism. 95 (7 Suppl 1): s1–s66. doi:10.1210/jc.2009-2509. PMC 6287288 . PMID 20566620.
- ↑ L'Hermite M (August 2013). "HRT optimization, using transdermal estradiol plus micronized progesterone, a safer HRT". Climacteric. 16 (Suppl 1): 44–53. doi:10.3109/13697137.2013.808563. PMID 23848491. S2CID 20401584.
- ↑ Fournier A, Fabre A, Mesrine S, Boutron-Ruault MC, Berrino F, Clavel-Chapelon F (March 2008). "Use of different postmenopausal hormone therapies and risk of histology- and hormone receptor-defined invasive breast cancer". Journal of Clinical Oncology. 26 (8): 1260–8. doi:10.1200/jco.2007.13.4338. PMC 2346534 . PMID 18323549.
- ↑ Harvard Women's Health Watch (August 2006). "What are bioidentical hormones?". Harvard Women's Health Watch. Retrieved 20 September 2014.
- ↑ Sicat BL, Brokaw DK (January 2004). "Nonhormonal alternatives for the treatment of hot flashes". Pharmacotherapy. 24 (1): 79–93. doi:10.1592/phco.24.1.79.34812. PMID 14740790. S2CID 22844064.
- ↑ Food and Drug Administration (28 June 2013). "FDA NEWS RELEASE: FDA approves the first non-hormonal treatment for hot flashes associated with menopause". FDA.
- ↑ "Apo-Clonidine - Uses, Side Effects, Interactions - Drug Factsheets - C-Health". chealth.canoe.com. Archived from the original on 22 December 2015. Retrieved 21 December 2015.
- ↑ "What Patients Need to Know About Hot Flashes". Medscape.(subscription required)
- ↑ Nissan HP, Lu J, Booth NL, Yamamura HI, Farnsworth NR, Wang ZJ (May 2007). "A red clover (Trifolium pratense) phase II clinical extract possesses opiate activity". Journal of Ethnopharmacology. 112 (1): 207–10. doi:10.1016/j.jep.2007.02.006. PMID 17350196.
- ↑ Wiklund IK, Mattsson LA, Lindgren R, Limoni C (1999). "Effects of a standardized ginseng extract on quality of life and physiological parameters in symptomatic postmenopausal women: a double-blind, placebo-controlled trial. Swedish Alternative Medicine Group". International Journal of Clinical Pharmacology Research. 19 (3): 89–99. PMID 10761538.
- ↑ Basch E, Bent S, Collins J, Dacey C, Hammerness P, Harrison M, et al. (2007). "Flax and flaxseed oil (Linum usitatissimum): a review by the Natural Standard Research Collaboration". Journal of the Society for Integrative Oncology. 5 (3): 92–105. PMID 17761128. S2CID 37254359.
- ↑ Bergman Jungeström M, Thompson LU, Dabrosin C (February 2007). "Flaxseed and its lignans inhibit estradiol-induced growth, angiogenesis, and secretion of vascular endothelial growth factor in human breast cancer xenografts in vivo". Clinical Cancer Research. 13 (3): 1061–7. doi: 10.1158/1078-0432.CCR-06-1651 . PMID 17289903.
- 1 2 Touillaud MS, Thiébaut AC, Fournier A, Niravong M, Boutron-Ruault MC, Clavel-Chapelon F (March 2007). "Dietary lignan intake and postmenopausal breast cancer risk by estrogen and progesterone receptor status". Journal of the National Cancer Institute. 99 (6): 475–86. doi:10.1093/jnci/djk096. PMC 2292813 . PMID 17374837.
- ↑ "Flaxseed in Treating Postmenopausal Women With Hot Flashes Who Have a History of Breast Cancer or Other Cancer or Who Do Not Wish to Take Estrogen Therapy". ClinicalTrials.gov. U.S. National Institute of Health. November 2010. Retrieved 20 April 2013.
- ↑ Frisk JW, Hammar ML, Ingvar M, Spetz Holm AC (May 2014). "How long do the effects of acupuncture on hot flashes persist in cancer patients?". Supportive Care in Cancer. 22 (5): 1409–15. doi:10.1007/s00520-014-2126-2. PMID 24477325. S2CID 9607095.
- ↑ Lee MS, Kim KH, Shin BC, Choi SM, Ernst E (July 2009). "Acupuncture for treating hot flushes in men with prostate cancer: a systematic review". Supportive Care in Cancer. 17 (7): 763–70. doi:10.1007/s00520-009-0589-3. PMID 19224253. S2CID 21847920.
- ↑ Messina M, Hughes C (2003). "Efficacy of soyfoods and soybean isoflavone supplements for alleviating menopausal symptoms is positively related to initial hot flush frequency". Journal of Medicinal Food. 6 (1): 1–11. doi:10.1089/109662003765184697. PMID 12804015.
- ↑ Lock M (May–August 1994). "Menopause in cultural context". Experimental Gerontology. 29 (3–4): 307–17. doi:10.1016/0531-5565(94)90011-6. PMID 7925751. S2CID 25719669.
- ↑ Lee, Emma; Anselmo, Miguel; Tahsin, Chowdhury Tasnova; Vanden Noven, Marnie; Stokes, William; Carter, Jason R.; Keller-Ross, Manda L. (1 December 2022). "Vasomotor symptoms of menopause, autonomic dysfunction, and cardiovascular disease". American Journal of Physiology. Heart and Circulatory Physiology. 323 (6): H1270–H1280. doi:10.1152/ajpheart.00477.2022. ISSN 1522-1539. PMC 9744645 . PMID 36367692.