Related Research Articles
Alternative medicine is any practice that aims to achieve the healing effects of medicine despite lacking biological plausibility,testability,repeatability,or evidence from clinical trials. Complementary medicine (CM),complementary and alternative medicine (CAM),integrated medicine or integrative medicine (IM),and holistic medicine attempt to combine alternative practices with those of mainstream medicine. Alternative therapies share in common that they reside outside of medical science and instead rely on pseudoscience. Traditional practices become "alternative" when used outside their original settings and without proper scientific explanation and evidence. Frequently used derogatory terms for relevant practices are new age or pseudo- medicine,with little distinction from quackery.

Hippocrates of Kos,also known as Hippocrates II,was a Greek physician of the classical period who is considered one of the most outstanding figures in the history of medicine. He is traditionally referred to as the "Father of Medicine" in recognition of his lasting contributions to the field,such as the use of prognosis and clinical observation,the systematic categorization of diseases,or the formulation of humoral theory. The Hippocratic school of medicine revolutionized ancient Greek medicine,establishing it as a discipline distinct from other fields with which it had traditionally been associated,thus establishing medicine as a profession.

The Hippocratic Oath is an oath of ethics historically taken by physicians. It is one of the most widely known of Greek medical texts. In its original form,it requires a new physician to swear,by a number of healing gods,to uphold specific ethical standards. The oath is the earliest expression of medical ethics in the Western world,establishing several principles of medical ethics which remain of paramount significance today. These include the principles of medical confidentiality and non-maleficence. As the seminal articulation of certain principles that continue to guide and inform medical practice,the ancient text is of more than historic and symbolic value. It is enshrined in the legal statutes of various jurisdictions,such that violations of the oath may carry criminal or other liability beyond the oath's symbolic nature.
Socialized medicine is a term used in the United States to describe and discuss systems of universal health care—medical and hospital care for all by means of government regulation of health care and subsidies derived from taxation. Because of historically negative associations with socialism in American culture,the term is usually used pejoratively in American political discourse. The term was first widely used in the United States by advocates of the American Medical Association in opposition to President Harry S. Truman's 1947 health care initiative. It was later used in opposition to Medicare. The Affordable Care Act has been described in terms of socialized medicine,but the act's objective is rather socialized insurance,not government ownership of hospitals and other facilities as is common in other nations.

A do-not-resuscitate order (DNR),also known as Do Not Attempt Resuscitation (DNAR),Do Not Attempt Cardiopulmonary Resuscitation (DNACPR),no code or allow natural death,is a medical order,written or oral depending on country,indicating that a person should not receive cardiopulmonary resuscitation (CPR) if that person's heart stops beating. Sometimes these decisions and the relevant documents also encompass decisions around other critical or life-prolonging medical interventions. The legal status and processes surrounding DNR orders vary from country to country. Most commonly,the order is placed by a physician based on a combination of medical judgement and patient involvement.
Internal medicine or general internal medicine is the medical specialty dealing with the prevention,diagnosis,and treatment of internal diseases. Doctors specializing in internal medicine are called internists,or physicians in Commonwealth nations. Internists are medical specialists that are skilled in the management of patients who have undifferentiated or multi-system disease processes. Internists care for hospitalized (inpatient) and ambulatory (outpatient) patients and may play a major role in teaching and research. Internists are qualified physicians with postgraduate training in internal medicine and should not be confused with "interns",a term for doctors in their first year of residency training.
Medical ethics is an applied branch of ethics which analyzes the practice of clinical medicine and related scientific research. Medical ethics is based on a set of values that professionals can refer to in the case of any confusion or conflict. These values include the respect for autonomy,non-maleficence,beneficence,and justice. Such tenets may allow doctors,care providers,and families to create a treatment plan and work towards the same common goal. It is important to note that these four values are not ranked in order of importance or relevance and that they all encompass values pertaining to medical ethics. However,a conflict may arise leading to the need for hierarchy in an ethical system,such that some moral elements overrule others with the purpose of applying the best moral judgement to a difficult medical situation. Medical ethics is particularly relevant in decisions regarding involuntary treatment and involuntary commitment.
Health law is a field of law that encompasses federal,state,and local law,rules,regulations and other jurisprudence among providers,payers and vendors to the health care industry and its patients,and delivery of health care services,with an emphasis on operations,regulatory and transactional issues.
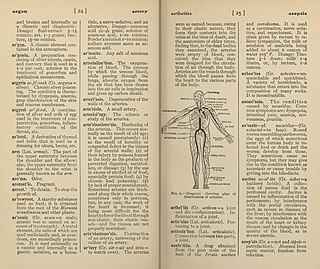
A medical dictionary is a lexicon for words used in medicine. The three major medical dictionaries in the United States are Stedman's,Taber's,and Dorland's. Other significant medical dictionaries are distributed by Elsevier. Dictionaries often have multiple versions,with content adapted for different user groups. For example Stedman's Concise Medical Dictionary and Dorland's are for general use and allied health care,while the full text editions are reference works used by medical students,doctors,and health professionals. Medical dictionaries are commonly available in print,online,or as downloadable software packages for personal computers and smartphones.

Arnold Seymour Relman —known as Bud Relman to intimates —was an American internist and professor of medicine and social medicine. He was editor of The New England Journal of Medicine (NEJM) from 1977 to 1991,where he instituted two important policies:one asking the popular press not to report on articles before publication and another requiring authors to disclose conflicts of interest. He wrote extensively on medical publishing and reform of the U.S. health care system,advocating non-profit delivery of single-payer health care. Relman ended his career as professor emeritus at Harvard Medical School in Boston,Massachusetts.

Ezekiel Jonathan "Zeke" Emanuel is an American oncologist,bioethicist and senior fellow at the Center for American Progress. He is the current Vice Provost for Global Initiatives at the University of Pennsylvania and chair of the Department of Medical Ethics and Health Policy. Previously,Emanuel served as the Diane and Robert Levy University Professor at Penn. He holds a joint appointment at the University of Pennsylvania School of Medicine and the Wharton School and was formerly an associate professor at the Harvard Medical School until 1998 when he joined the National Institutes of Health.

Medicine in ancient Rome was highly influenced by ancient Greek medicine,but also developed new practices through knowledge of the Hippocratic Corpus combined with use of the treatment of diet,regimen,along with surgical procedures. This was most notably seen through the works of two of the prominent Greek physicians,Dioscorides and Galen,who practiced medicine and recorded their discoveries. This is contrary to two other physicians like Soranus of Ephesus and Asclepiades of Bithynia,who practiced medicine both in outside territories and in ancient Roman territory,subsequently. Dioscorides was a Roman army physician,Soranus was a representative for the Methodic school of medicine,Galen performed public demonstrations,and Asclepiades was a leading Roman physician. These four physicians all had knowledge of medicine,ailments,and treatments that were healing,long lasting and influential to human history.
The doctor–patient relationship is a central part of health care and the practice of medicine. A doctor–patient relationship is formed when a doctor attends to a patient's medical needs and is usually through consent. This relationship is built on trust,respect,communication,and a common understanding of both the doctor and patients' sides. The trust aspect of this relationship goes is mutual:the doctor trusts the patient to reveal any information that may be relevant to the case,and in turn,the patient trusts the doctor to respect their privacy and not disclose this information to outside parties.

Narrative Medicine is the discipline of applying the skills used in analyzing literature to interviewing patients. The premise of narrative medicine is that how a patient speaks about his or her illness or complaint is analogous to how literature offers a plot with characters and is filled with metaphors,and that becoming conversant with the elements of literature facilitates understanding the stories that patients bring. Narrative Medicine is a diagnostic and comprehensive approach that utilizes patients' narratives in clinical practice,research,and education to promote healing. Beyond attempts to reach accurate diagnoses,it aims to address the relational and psychological dimensions that occur in tandem with physical illness. Narrative medicine aims not only to validate the experience of the patient,it also encourages creativity and self-reflection in the physician.
Healthcare rationing in the United States exists in various forms. Access to private health insurance is rationed on price and ability to pay. Those unable to afford a health insurance policy are unable to acquire a private plan except by employer-provided and other job-attached coverage,and insurance companies sometimes pre-screen applicants for pre-existing medical conditions. Applicants with such conditions may be declined cover or pay higher premiums and/or have extra conditions imposed such as a waiting period.

Choosing Wisely is a United States-based health educational campaign,led by the ABIM Foundation,about unnecessary health care.
Health policy and management is the field relating to leadership,management,and administration of public health systems,health care systems,hospitals,and hospital networks. Health care administrators are considered health care professionals.

M. R. Rajagopal is an Indian palliative care physician referred to as the 'father of palliative care in India' in honour of his significant contribution to the palliative care scene in India.
Eric Jonathan Cassell was an American physician and bioethicist.
William Francis May is an American ethicist.
References
- ↑ Engagement, Office of the Vice President for Global. "Maxwell Gregg Bloche". global.georgetown.edu. Retrieved 2022-05-28.
- ↑ Pasquale, Frank (October 2011). "The Hippocratic Myth: Why doctors are under pressure to ration care, practice politics, and compromise their promise to heal". Journal of Legal Medicine. 32 (4): 529–545. doi:10.1080/01947648.2011.632724. S2CID 73147942.
- ↑ Bloche, M. Gregg (2017-08-12). "Opinion | When Torture Becomes Science". The New York Times. ISSN 0362-4331 . Retrieved 2022-05-28.
- 1 2 "M. Gregg Bloche" . Retrieved 2022-05-28.
- ↑ "Bookshelf | Columbia College Today". www.college.columbia.edu. Retrieved 2022-05-28.
- ↑ Bloche, M. (1996-01-01). "Beyond Autonomy: Coersion and Morality in Clinical Relationships". Health Matrix: The Journal of Law-Medicine. 6 (2): 229. ISSN 0748-383X.
- ↑ Bloche, M. Gregg (2016-11-22). "Opinion | When Doctors First Do Harm". The New York Times. ISSN 0362-4331 . Retrieved 2022-05-28.
- ↑ "Toward a Science of Torture?". Texas Law Review. 2017-05-16. Retrieved 2022-05-28.
- ↑ "M. Gregg Bloche". John Simon Guggenheim Memorial Foundation. Retrieved 2022-05-28.
- ↑ Adrian, Chris (May 13, 2011). "M. Gregg Bloche's "The Hippocratic Myth"". The Washington Post. Retrieved May 27, 2022.
- ↑ Sessions, Samuel Y. (2011-08-24). "The Hippocratic Myth: Why Doctors Are Under Pressure to Ration Care, Practice Politics, and Compromise Their Promise to Heal". JAMA. 306 (8): 883–884. doi:10.1001/jama.2011.1215. ISSN 0098-7484.