
The European Medicines Agency (EMA) is an agency of the European Union (EU) in charge of the evaluation and supervision of pharmaceutical products. Prior to 2004, it was known as the European Agency for the Evaluation of Medicinal Products or European Medicines Evaluation Agency (EMEA).
The Therapeutic Goods Administration (TGA) is the medicine and therapeutic regulatory agency of the Australian Government. As part of the Department of Health and Aged Care, the TGA regulates the quality, supply and advertising of medicines, pathology devices, medical devices, blood products and most other therapeutics. Any items that claim to have a therapeutic effect, are involved in the administration of medication, or are otherwise covered by the Therapeutic Goods Act 1989, the Therapeutic Goods Regulations 1990, or a ministerial order, must be approved by the TGA and registered in the Australian Register of Therapeutic Goods.
The Joint Committee on Vaccination and Immunisation (JCVI) is an independent expert advisory committee that advises United Kingdom health departments on immunisation, making recommendations concerning vaccination schedules and vaccine safety. It has a statutory role in England and Wales, and health departments in Scotland and Northern Ireland may choose to accept its advice.
A COVID‑19 vaccine is a vaccine intended to provide acquired immunity against severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the virus that causes coronavirus disease 2019 (COVID‑19).

The Moderna COVID‑19 vaccine, sold under the brand name Spikevax, is a COVID-19 vaccine developed by the American company Moderna, the United States National Institute of Allergy and Infectious Diseases (NIAID), and the Biomedical Advanced Research and Development Authority (BARDA). Depending on the jurisdiction, it is authorized for use in humans aged six months, twelve years, or eighteen years and older. It provides protection against COVID-19, which is caused by infection by the SARS-CoV-2 virus. It is designed to be administered in two or three 0.5-mL doses given by intramuscular injection at an interval of at least 28 days apart.

BioNTech SE is a German biotechnology company based in Mainz that develops and manufactures active immunotherapies for patient-specific approaches to the treatment of diseases. It develops pharmaceutical candidates based on messenger ribonucleic acid (mRNA) for use as individualized cancer immunotherapies, as vaccines against infectious diseases and as protein replacement therapies for rare diseases, and also engineered cell therapy, novel antibodies and small molecule immunomodulators as treatment options for cancer.
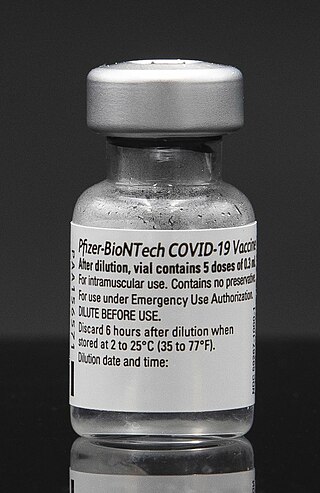
The Pfizer–BioNTech COVID-19 vaccine, sold under the brand name Comirnaty, is an mRNA-based COVID-19 vaccine developed by the German biotechnology company BioNTech. For its development, BioNTech collaborated with the American company Pfizer to carry out clinical trials, logistics, and manufacturing. It is authorized for use in humans to provide protection against COVID-19, caused by infection with the SARS-CoV-2 virus. The vaccine is given by intramuscular injection. It is composed of nucleoside-modified mRNA (modRNA) encoding a mutated form of the full-length spike protein of SARS-CoV-2, which is encapsulated in lipid nanoparticles. Initial advice indicated that vaccination required two doses given 21 days apart, but the interval was later extended to up to 42 days in the US, and up to four months in Canada.

Dame June Munro Raine, is a British doctor who is currently serving as the Chief Executive Officer of the Medicines and Healthcare products Regulatory Agency (MHRA) in the United Kingdom. Raine spent much of her career in the Medicines Division of the MHRA.

V451 was a COVID-19 vaccine candidate developed by the University of Queensland and the Australian pharmaceutical company CSL Limited. The vaccine candidate used the University of Queensland's molecular clamp technology and the MF59 adjuvant.

The Human Medicines (Amendment) Regulations 2020 is a statutory instrument (SI) that was laid before Parliament on 16 October 2020 to make provision for the strengthening of existing regulations that allow for the temporary authorisation of the supply of unlicensed medicines, including vaccines, in response to certain public health threats, and for the expansion of the workforce able to administer the COVID-19 vaccines and influenza vaccines. Certain amendments within the instrument, regulations 3, 12 and 3, allowing for the administration of vaccines by a wider range of medically trained people such as an "occupational health vaccinator" are time-limited to 1 April 2022.
The COVID-19 vaccination programme in the United Kingdom is an ongoing mass immunisation campaign for coronavirus disease 2019 (COVID-19) during the COVID-19 pandemic in the United Kingdom.

ALC-0315 is a synthetic lipid. A colorless oily material, it has attracted attention as a component of the SARS-CoV-2 vaccine, BNT162b2, from BioNTech and Pfizer. Specifically, it is one of four components that form lipid nanoparticles (LNPs), which encapsulate and protect the otherwise fragile mRNA that is the active ingredient in these drugs. These nanoparticles promote the uptake of therapeutically effective nucleic acids such as oligonucleotides or mRNA both in vitro and in vivo.

Valneva COVID-19 vaccine is a COVID-19 vaccine developed by French biotechnology company Valneva SE in collaboration with the American biopharmaceutical company Dynavax Technologies.

The National Health Regulatory Authority (NHRA) is an independent regulatory body established in 2010, under Law No. 38 of 2009, of the Kingdom of Bahrain.

SARS-CoV-2, the virus that causes COVID-19, was isolated in late 2019. Its genetic sequence was published on 11 January 2020, triggering an urgent international response to prepare for an outbreak and hasten the development of a preventive COVID-19 vaccine. Since 2020, vaccine development has been expedited via unprecedented collaboration in the multinational pharmaceutical industry and between governments. By June 2020, tens of billions of dollars were invested by corporations, governments, international health organizations, and university research groups to develop dozens of vaccine candidates and prepare for global vaccination programs to immunize against COVID‑19 infection. According to the Coalition for Epidemic Preparedness Innovations (CEPI), the geographic distribution of COVID‑19 vaccine development shows North American entities to have about 40% of the activity, compared to 30% in Asia and Australia, 26% in Europe, and a few projects in South America and Africa.

A dispute broke out in January 2021 between the European Commission and the pharmaceutical company AstraZeneca AB about the provision of COVID-19 vaccines during the COVID-19 pandemic, and, in February, spilled out into a dispute over Article 16 of the Northern Ireland Protocol. Vaccination proceeded apace in the UK but more slowly in the EU, and by the end of March 2021, over 30% of the UK population had received at least one dose of vaccine compared to about 8% of the EU population. This was partly due to limited availability of the AstraZeneca vaccine in the EU. The World Health Organization and the European Medicines Agency continued to state that the vaccine was safe and effective. However, a representative of the European Medicines Agency said in June that vaccines based on the mRNA technology should be preferred if available for all age groups, including for the over 60s.

The COVID-19 vaccination programme in the Republic of Ireland is an ongoing mass immunisation campaign that began on 29 December 2020 in response to the COVID-19 pandemic in the Republic of Ireland. Ireland's vaccination rollout has been praised as one of the most successful rollouts in the world and was ranked number one in the European Union in terms of its percentage of adult population fully vaccinated, and was also ranked number one in the EU for the number of booster vaccines administered.

Post-vaccination embolic and thrombotic events, termed vaccine-induced immune thrombotic thrombocytopenia (VITT), vaccine-induced prothrombotic immune thrombocytopenia (VIPIT), thrombosis with thrombocytopenia syndrome (TTS), vaccine-induced immune thrombocytopenia and thrombosis (VITT), or vaccine-associated thrombotic thrombocytopenia (VATT), are rare types of blood clotting syndromes that were initially observed in a number of people who had previously received the Oxford–AstraZeneca COVID‑19 vaccine (AZD1222) during the COVID‑19 pandemic. It was subsequently also described in the Janssen COVID‑19 vaccine, leading to the suspension of its use until its safety had been reassessed. On 5 May 2022 the FDA posted a bulletin limiting the use of the Janssen Vaccine to very specific cases due to further reassessment of the risks of TTS, although the FDA also stated in the same bulletin that the benefits of the vaccine outweigh the risks.

The COVID-19 vaccination in Singapore is an ongoing immunisation campaign against severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the virus that causes coronavirus disease 2019 (COVID-19), in response to the ongoing pandemic in the country. Singapore has a very high vaccination rate, with more than 92% of its total population having completed their vaccination regimen.















