
Universal precautions refers to the practice, in medicine, of avoiding contact with patients' bodily fluids, by means of the wearing of nonporous articles such as medical gloves, goggles, and face shields. The practice was introduced in 1985–88. In 1987, the practice of universal precautions was adjusted by a set of rules known as body substance isolation. In 1996, both practices were replaced by the latest approach known as standard precautions. Use of personal protective equipment is now recommended in all health settings.

A biosafety level (BSL) is a set of biocontainment precautions required to isolate dangerous biological agents in an enclosed laboratory facility. The levels of containment range from the lowest biosafety level 1 (BSL-1) to the highest at level 4 (BSL-4). In the United States, the Centers for Disease Control and Prevention (CDC) have specified these levels. In the European Union, the same biosafety levels are defined in a directive. In Canada the four levels are known as Containment Levels. Facilities with these designations are also sometimes given as P1 through P4, as in the term "P3 laboratory".

Hygiene is a series of practices performed to preserve health. According to the World Health Organization (WHO), "Hygiene refers to conditions and practices that help to maintain health and prevent the spread of diseases." Personal hygiene refers to maintaining the body's cleanliness.
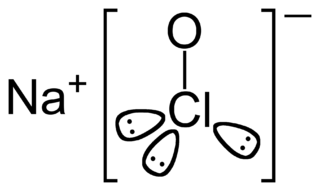
Sodium hypochlorite is a chemical compound with the formula NaOCl or NaClO, comprising a sodium cation and a hypochlorite anion. It may also be viewed as the sodium salt of hypochlorous acid. The anhydrous compound is unstable and may decompose explosively. It can be crystallized as a pentahydrate NaOCl·5H
2O, a pale greenish-yellow solid which is not explosive and is stable if kept refrigerated.
A blood-borne disease is a disease that can be spread through contamination by blood and other body fluids. Blood can contain pathogens of various types, chief among which are microorganisms, like bacteria and parasites, and non-living infectious agents such as viruses. Three bloodborne pathogens in particular, all viruses, are cited as of primary concern to health workers by the CDC-NIOSH: HIV, hepatitis B (HVB), & hepatitis C (HVC).

An operating theater is a facility within a hospital where surgical operations are carried out in an aseptic environment.

Disinfectants are antimicrobial agents designed to inactivate or destroy microorganisms on inert surfaces. Disinfection does not necessarily kill all microorganisms, especially resistant bacterial spores; it is less effective than sterilization, which is an extreme physical and/or chemical process that kills all types of life. Disinfectants are different from other antimicrobial agents such as antibiotics, which destroy microorganisms within the body, and antiseptics, which destroy microorganisms on living tissue. Disinfectants are also different from biocides — the latter are intended to destroy all forms of life, not just microorganisms. Disinfectants work by destroying the cell wall of microbes or interfering with their metabolism.

Dishwashing or dish washing, also known as washing up, is the process of cleaning cooking utensils, dishes, cutlery and other items to prevent foodborne illness. This is either achieved by hand in a sink using dishwashing detergent or by using a dishwasher and may take place in a kitchen, utility room, scullery or elsewhere. In Britain to do the washing up also includes to dry and put away. There are cultural divisions over rinsing and drying after washing.

A hospital-acquired infection (HAI), also known as a nosocomial infection, is an infection that is acquired in a hospital or other health care facility. To emphasize both hospital and nonhospital settings, it is sometimes instead called a health care–associated infection. Such an infection can be acquired in hospital, nursing home, rehabilitation facility, outpatient clinic, diagnostic laboratory or other clinical settings. Infection is spread to the susceptible patient in the clinical setting by various means. Health care staff also spread infection, in addition to contaminated equipment, bed linens, or air droplets. The infection can originate from the outside environment, another infected patient, staff that may be infected, or in some cases, the source of the infection cannot be determined. In some cases the microorganism originates from the patient's own skin microbiota, becoming opportunistic after surgery or other procedures that compromise the protective skin barrier. Though the patient may have contracted the infection from their own skin, the infection is still considered nosocomial since it develops in the health care setting.

Viral hemorrhagic fevers (VHFs) are a diverse group of animal and human illnesses in which fever and hemorrhage are caused by a viral infection. VHFs may be caused by five distinct families of RNA viruses: the families Arenaviridae, Filoviridae, Bunyaviridae, Flaviviridae, and Rhabdoviridae. All types of VHF are characterized by fever and bleeding disorders and all can progress to high fever, shock and death in many cases. Some of the VHF agents cause relatively mild illnesses, such as the Scandinavian nephropathia epidemica, while others, such as Ebola virus, can cause severe, life-threatening disease.
Asepsis is the state of being free from disease-causing micro-organisms. The term often refers to those practices used to promote or induce asepsis in an operative field of surgery or medicine to prevent infection.
Infection control is the discipline concerned with preventing nosocomial or healthcare-associated infection, a practical sub-discipline of epidemiology. It is an essential, though often underrecognized and undersupported, part of the infrastructure of health care. Infection control and hospital epidemiology are akin to public health practice, practiced within the confines of a particular health-care delivery system rather than directed at society as a whole. Anti-infective agents include antibiotics, antibacterials, antifungals, antivirals and antiprotozoals.

Matthew Lukwiya was a Ugandan physician and the supervisor of St. Mary's Hospital Lacor, outside of Gulu. He was at the forefront of the 2000 Ebola virus disease outbreak in Uganda.
Biomedical waste/hospital waste is any kind of waste containing infectious materials. It may also include waste associated with the generation of biomedical waste that visually appears to be of medical or laboratory origin, as well research laboratory waste containing biomolecules or organisms that are mainly restricted from environmental release. As detailed below, discarded sharps are considered biomedical waste whether they are contaminated or not, due to the possibility of being contaminated with blood and their propensity to cause injury when not properly contained and disposed of. Biomedical waste is a type of biowaste.

In health care facilities, isolation represents one of several measures that can be taken to implement infection control: the prevention of contagious diseases from being spread from a patient to other patients, health care workers, and visitors, or from outsiders to a particular patient. Various forms of isolation exist, in some of which contact procedures are modified, and others in which the patient is kept away from all others. In a system devised, and periodically revised, by the U.S. Centers for Disease Control and Prevention (CDC), various levels of patient isolation comprise application of one or more formally described "precaution".

Scrubs are the sanitary clothing worn by surgeons, nurses, physicians and other workers involved in patient care in hospitals. Originally designed for use by surgeons and other operating room personnel, who would put them on when sterilizing themselves, or "scrubbing in", before surgery, they are now worn by many hospital personnel. Their use has been extended outside hospitals as well, to work environments where clothing may come into contact with infectious agents. Scrubs are designed to be simple, easy to launder, and cheap to replace if damaged or stained irreparably. In the United Kingdom, scrubs are sometimes known as theatre blues.
Precautionary statements form part of the Globally Harmonized System of Classification and Labelling of Chemicals (GHS). They are intended to form a set of standardized phrases giving advice about the correct handling of chemical substances and mixtures, which can be translated into different languages. As such, they serve the same purpose as the well-known S-phrases, which they are intended to replace.
Barrier nursing is a largely archaic term for a set of stringent infection control techniques used in nursing. The aim of barrier nursing is to protect medical staff against infection by patients and also protect patients with highly infectious diseases from spreading their pathogens to other non-infected people.

Chlorine-releasing compounds, also known as chlorine base compounds, are a family of chemicals that release chlorine. They are widely used to disinfect water, medical equipment, and surface areas as well as bleaching materials such as cloth. The presence of organic matter can make them less effective as disinfectants. They come as a powder that is mixed with water before use.
Single-use medical devices include any medical equipment, instrument or apparatus having the ability to only be used once in a hospital or clinic and then disposed. The Food and Drug Administration defines this as any device entitled by its manufacturer that it is intended use is for one single patient and one procedure only. It is not reusable, therefore has a short lifespan, and is limited to one patient. There are countless types of single use medical devices, ranging from external, such as plastic gumboots, gloves and bandages merely used to assist a patient to more complex and internal devices, consisting of sharp blades, needles and tubes. Both these devices are single used, because of multiple reasons, but mainly, as it came in contact with radioactivity, blood, infection and disease or human tissue and must therefore be terminated. Each country has its own strict legislation regarding medical waste and the reprocessing of medical devices in hospitals and clinics.




















