This article may require cleanup to meet Wikipedia's quality standards. The specific problem is: This article may be unbalanced to certain viewpoints, in particular, it does not clearly state the controversy surrounding the topic (see talk page).(June 2021) |
| Shaken baby syndrome | |
|---|---|
| Other names | abusive head trauma, non-accidental head injury, non-accidental trauma |
 | |
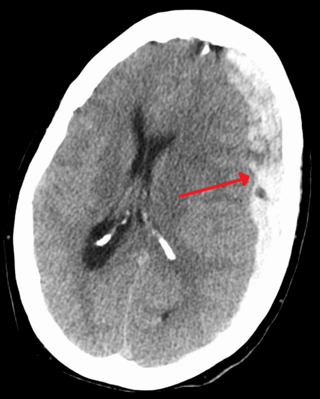
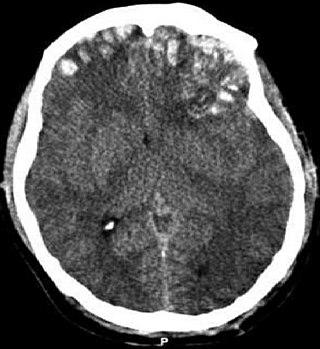
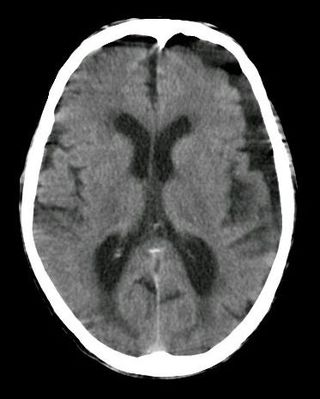
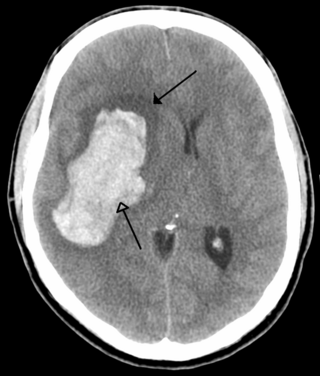
| An intraparenchymal bleed with overlying skull fracture from shaken baby syndrome | |
| Specialty | Pediatrics |
| Symptoms | Variable [1] |
| Complications | Seizures, visual impairment, cerebral palsy, cognitive impairment [2] [1] |
| Usual onset | Less than 5 years old [3] |
| Causes | Blunt trauma, vigorous shaking [1] |
| Diagnostic method | CT scan [1] |
| Prevention | Educating new parents [1] |
| Prognosis | Long term health problems common [3] |
| Frequency | 3 per 10,000 babies per year (US) [1] |
| Deaths | ≈25% risk of death [3] |
Shaken baby syndrome (SBS), also known as abusive head trauma (AHT), is a medical condition in children younger than five years old, [3] generally caused by blunt trauma, vigorous shaking, or a combination of both. [1] SBS is the leading cause of fatal head injuries in children under two, [4] with a risk of death of about 25%. [3] The most common symptoms include retinal bleeds, multiple fractures of the long bones, and subdural hematomas (bleeding in the brain). [5]
Contents
- Risk factors
- Mechanism
- Force
- Diagnosis
- Triad
- Classification
- Differential diagnosis
- Prevention
- Treatment
- Prognosis
- Epidemiology
- History
- Legal issues
- See also
- References
- External links
The condition is often caused as a result of a parent or caregiver becoming frustrated due to the child crying. [3] Diagnosis can be difficult as symptoms may be nonspecific. [1] A CT scan of the head is typically recommended if a concern is present. [1] If there are concerning findings on the CT scan, a full work-up for child abuse should occur, including an eye exam and skeletal survey. Retinal hemorrhage is highly associated with AHT, occurring in 78% of cases of AHT versus 5% of cases of non-abusive head trauma. [6] [7]
Diagnosing the syndrome has proven to be both challenging and contentious for medical professionals because objective witnesses to the initial trauma are generally unavailable. [8] This is said to be particularly problematic when the trauma is deemed 'non-accidental'. [9] Some medical professionals propose that SBS is the result of respiratory abnormalities leading to hypoxia and swelling of the brain. [10] The courtroom has become a forum for conflicting theories with which generally accepted medical literature has not been reconciled. [4] Often there are no outwardly visible signs of trauma, despite the presence of severe internal brain and eye injury. [1] Complications include seizures, visual impairment, cerebral palsy, cognitive impairment, and death. [2] [1]
Educating new parents appears to be beneficial in decreasing rates of the condition. [1] SBS is estimated to occur in three to four per 10,000 babies a year. [1] These signs have evolved through the years as accepted and recognized signs of child abuse. Medical professionals strongly suspect shaking as the cause of injuries when a young child presents with retinal bleed, fractures, soft tissue injuries, or subdural hematoma that cannot be explained by accidental trauma or other medical conditions. [11]
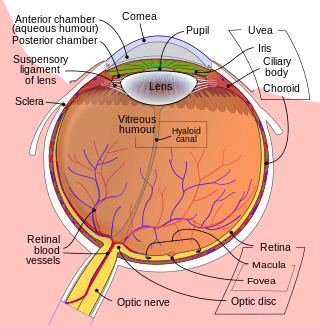
Retinal hemorrhage (bleeding) occurs in around 85% of SBS cases and the severity of retinal hemorrhage correlates with severity of head injury. [6] The type of retinal bleeds are often believed to be particularly characteristic of this condition, making the finding useful in establishing the diagnosis. [12]
Fractures of the vertebrae, long bones, and ribs may also be associated with SBS. [13] Dr. John Caffey reported in 1972 that metaphyseal avulsions (small fragments of bone torn off where the periosteum covering the bone and the cortical bone are tightly bound together) and "bones on both the proximal and distal sides of a single joint are affected, especially at the knee". [14]
Infants may display irritability, failure to thrive, alterations in eating patterns, lethargy, vomiting, seizures, bulging or tense fontanels (the soft spots on a baby's head), increased size of the head, altered breathing, and dilated pupils.