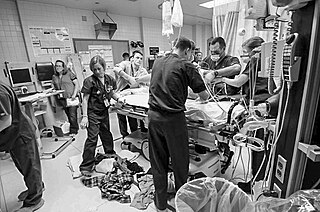
Emergency medicine is the medical speciality concerned with the care of illnesses or injuries requiring immediate medical attention. Emergency physicians specialize in providing care for unscheduled and undifferentiated patients of all ages. As first-line providers, in coordination with emergency medical services, they are primarily responsible for initiating resuscitation and stabilization and performing the initial investigations and interventions necessary to diagnose and treat illnesses or injuries in the acute phase. Emergency medical physicians generally practice in hospital emergency departments, pre-hospital settings via emergency medical services, and intensive care units. Still, they may also work in primary care settings such as urgent care clinics.

An emergency department (ED), also known as an accident and emergency department (A&E), emergency room (ER), emergency ward (EW) or casualty department, is a medical treatment facility specializing in emergency medicine, the acute care of patients who present without prior appointment; either by their own means or by that of an ambulance. The emergency department is usually found in a hospital or other primary care center.
Internal medicine, also known as general internal medicine in Commonwealth nations, is a medical specialty for medical doctors focused on the prevention, diagnosis, and treatment of internal diseases in adults. Medical practitioners of internal medicine are referred to as internists, or physicians in Commonwealth nations. Internists possess specialized skills in managing patients with undifferentiated or multi-system disease processes. They provide care to both hospitalized (inpatient) and ambulatory (outpatient) patients and often contribute significantly to teaching and research. Internists are qualified physicians who have undergone postgraduate training in internal medicine, and should not be confused with "interns", a term commonly used for a medical doctor who has obtained a medical degree but does not yet have a license to practice medicine unsupervised.
A patient is any recipient of health care services that are performed by healthcare professionals. The patient is most often ill or injured and in need of treatment by a physician, nurse, optometrist, dentist, veterinarian, or other health care provider.

A clinic is a health facility that is primarily focused on the care of outpatients. Clinics can be privately operated or publicly managed and funded. They typically cover the primary care needs of populations in local communities, in contrast to larger hospitals which offer more specialized treatments and admit inpatients for overnight stays.

Telehealth is the distribution of health-related services and information via electronic information and telecommunication technologies. It allows long-distance patient and clinician contact, care, advice, reminders, education, intervention, monitoring, and remote admissions. Telemedicine is sometimes used as a synonym, or is used in a more limited sense to describe remote clinical services, such as diagnosis and monitoring. When rural settings, lack of transport, a lack of mobility, conditions due to outbreaks, epidemics or pandemics, decreased funding, or a lack of staff restrict access to care, telehealth may bridge the gap as well as provide distance-learning; meetings, supervision, and presentations between practitioners; online information and health data management and healthcare system integration. Telehealth could include two clinicians discussing a case over video conference; a robotic surgery occurring through remote access; physical therapy done via digital monitoring instruments, live feed and application combinations; tests being forwarded between facilities for interpretation by a higher specialist; home monitoring through continuous sending of patient health data; client to practitioner online conference; or even videophone interpretation during a consult.

Telenursing refers to the use of information technology in the provision of nursing services whenever physical distance exists between patient and nurse, or between any number of nurses. As a field, it is part of telemedicine, and has many points of contacts with other medical and non-medical applications, such as telediagnosis, teleconsultation, and telemonitoring. The field, however, is still being developed as the information on telenursing isn't comprehensive enough.

Montefiore Medical Center is a premier academic medical center and the primary teaching hospital of the Albert Einstein College of Medicine in the Bronx, New York City. Its main campus, the Henry and Lucy Moses Division, is located in the Norwood section of the northern Bronx. It is named for Moses Montefiore and is one of the 50 largest employers in New York. In 2020, Montefiore was ranked No. 6 New York City metropolitan area hospitals by U.S. News & World Report. Adjacent to the main hospital is the Children's Hospital at Montefiore, which serves infants, children, teens, and young adults aged 0–21.

Los Angeles County Department of Health Services operates the public hospitals and clinics in Los Angeles County, and is the United States' second largest municipal health system, after NYC Health + Hospitals.
Acute care is a branch of secondary health care where a patient receives active but short-term treatment for a severe injury or episode of illness, an urgent medical condition, or during recovery from surgery. In medical terms, care for acute health conditions is the opposite from chronic care, or longer-term care.
Home automation for the elderly and disabled focuses on making it possible for older adults and people with disabilities to remain at home, safe and comfortable. Home automation is becoming a viable option for older adults and people with disabilities who would prefer to stay in the comfort of their homes rather than move to a healthcare facility. This field uses much of the same technology and equipment as home automation for security, entertainment, and energy conservation but tailors it towards old people and people with disabilities.
The medical home, also known as the patient-centered medical home (PCMH), is a team-based health care delivery model led by a health care provider to provide comprehensive and continuous medical care to patients with a goal to obtain maximal health outcomes. It is described in the "Joint Principles" as "an approach to providing comprehensive primary care for children, youth and adults."
In medicine, describing a disease as acute denotes that it is of recent onset; it occasionally denotes a short duration. The quantification of how much time constitutes "short" and "recent" varies by disease and by context, but the core denotation of "acute" is always qualitatively in contrast with "chronic", which denotes long-lasting disease.
Disease or patient registries are collections of secondary data related to patients with a specific diagnosis, condition, or procedure, and they play an important role in post marketing surveillance of pharmaceuticals. Registries are different from indexes in that they contain more extensive data.
Teledermatology is a subspecialty in the medical field of dermatology and probably one of the most common applications of telemedicine and e-health. In teledermatology, telecommunication technologies are used to exchange medical information over a distance using audio, visual, and data communication. Applications comprise health care management such as diagnoses, consultation, and treatment as well as (continuous) education.

Remote patient monitoring (RPM) is a technology to enable monitoring of patients outside of conventional clinical settings, such as in the home or in a remote area, which may increase access to care and decrease healthcare delivery costs. RPM involves the constant remote care of patients by their physicians, often to track physical symptoms, chronic conditions, or post-hospitalization rehab.
Telehomecare (THC) is a subfield within telehealth. It involves the delivery of healthcare services to patients at home through the use of telecommunications technologies, which enable the interaction of voice, video, and health-related data. The management of care is done from an external site by a healthcare professional.
Patient satisfaction is a measure of the extent to which a patient is content with the health care which they received from their health care provider.
Travel health nursing is a nursing specialty which promotes the health and safety of national and international travelers. Similar to travel medicine, it is an interdisciplinary practice which draws from the knowledge bases of vaccines, epidemiology, tropical medicine, public health, and health education. Travel nursing has experienced an increase in global demand due to the evolution of travel medicine. Travel health nursing was recognized during the 1980s as an emerging occupation to meet the needs of the traveling public, and additional education and training was established. Travel health nurses typically work in "private practice, hospital outpatient units, universities, the government, and the military", and have more opportunities and leadership roles as travel has become more common. However, they also experience organizational and support-related conflicts with general practitioners and patients in healthcare settings.
Opioid tapering is the reduction of opioid doses over time. Opioid tapering is typically done in people taking opioids for chronic pain. Tapering may be conducted in medically-supervised inpatient or outpatient settings.










