
Major depressive disorder (MDD), also known as clinical depression, is a mental disorder characterized by at least two weeks of pervasive low mood, low self-esteem, and loss of interest or pleasure in normally enjoyable activities. Introduced by a group of US clinicians in the mid-1970s, the term was adopted by the American Psychiatric Association for this symptom cluster under mood disorders in the 1980 version of the Diagnostic and Statistical Manual of Mental Disorders (DSM-III), and has become widely used since.

Ketamine is a dissociative anesthetic used medically for induction and maintenance of anesthesia. It is also used as a treatment for depression and pain management. Ketamine is a novel compound that was derived from phencyclidine in 1962 in pursuit of a safer anesthetic with fewer hallucinogenic effects.
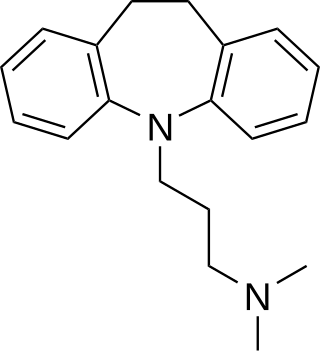
Imipramine, sold under the brand name Tofranil, among others, is a tricyclic antidepressant (TCA) mainly used in the treatment of depression. It is also effective in treating anxiety and panic disorder. Imipramine is taken by mouth.
Biological psychiatry or biopsychiatry is an approach to psychiatry that aims to understand mental disorder in terms of the biological function of the nervous system. It is interdisciplinary in its approach and draws on sciences such as neuroscience, psychopharmacology, biochemistry, genetics, epigenetics and physiology to investigate the biological bases of behavior and psychopathology. Biopsychiatry is the branch of medicine which deals with the study of the biological function of the nervous system in mental disorders.
Treatment-resistant depression is a term used in psychiatry to describe people with major depressive disorder (MDD) who do not respond adequately to a course of appropriate antidepressant medication within a certain time. Definitions of treatment-resistant depression vary, and they do not include a resistance to psychological therapies. Inadequate response has most commonly been defined as less than 50% reduction in depressive symptoms following treatment with at least one antidepressant medication, although definitions vary widely. Some other factors that may contribute to inadequate treatment are: a history of repeated or severe adverse childhood experiences, early discontinuation of treatment, insufficient dosage of medication, patient noncompliance, misdiagnosis, cognitive impairment, low income and other socio-economic variables, and concurrent medical conditions, including comorbid psychiatric disorders. Cases of treatment-resistant depression may also be referred to by which medications people with treatment-resistant depression are resistant to. In treatment-resistant depression adding further treatments such as psychotherapy, lithium, or aripiprazole is weakly supported as of 2019.

Cycloserine, sold under the brand name Seromycin, is a GABA transaminase inhibitor and an antibiotic, used to treat tuberculosis. Specifically it is used, along with other antituberculosis medications, for active drug resistant tuberculosis. It is given by mouth.
The emphasis of the treatment of bipolar disorder is on effective management of the long-term course of the illness, which can involve treatment of emergent symptoms. Treatment methods include pharmacological and psychological techniques.
Helen S. Mayberg was born in 1956 in California. She is an American neurologist. Mayberg is known in particular for her work delineating abnormal brain function in patients with major depression using functional neuroimaging. This work led to the first pilot study of deep brain stimulation (DBS), a reversible method of selective modulation of a specific brain circuit, for patients with treatment-resistant depression. As of August 2019, she has published 211 original peer-reviewed articles, 31 books and book chapters, and acted as principal investigator on 24 research grants. Mayberg is coinventor with Andres Lozano of “Method for Treating Depression Mood Disorders and Anxiety Disorders using Neuromodulation,” US patent 2005/0033379A1. St. Jude Medical Neuromodulation licensed her intellectual property to develop Subcallosal Cingulate Deep Brain Stimulation for Treatment-Resistant Unipolar and Bipolar Depression for the treatment of severe depression. As of 2018, Mayberg holds positions as Professor of Neurology and Neurosurgery and Professor, Psychiatry and Neuroscience, both at Mount Sinai Medical School, and Professor of Psychiatry, Emory University; Emory University Hospital. Since 2018, she has served as Director, Nash Family Center for Advanced Circuit Therapeutics at the Icahn School of Medicine at Mount Sinai.
GABA gamma-aminobutyric acid (GABA) is a key chemical messenger or a neurotransmitter in the central nervous system, that significantly inhibits neuronal transmission. GABA calms the brain and controls several physiological processes, such as stress, anxiety, and sleep. GABAA receptors are a class of ionotropic receptors that are triggered by GABA. They are made up of five subunits that are assembled in various configurations to create distinct receptor subtypes. The direct influx of chloride ions causes rapid inhibitory responses. GABAB receptors are another type of metabotropic receptor that modifies intracellular signaling pathways to provide slower, sustained inhibitory responses. At synapses, GABAA receptors facilitate rapid inhibitory neurotransmission, whereas GABAB receptor which comprise GABA B1 and GABA B2 subunits—control neurotransmitter release and cellular excitability over a longer period of time. As these. These unique qualities help explain the various ways that GABAergic neurotransmission controls brain communication and neuronal function.

Esketamine, also known as (S)-ketamine or S(+)-ketamine, is the S(+) enantiomer of ketamine. It is a dissociative hallucinogen drug used as a general anesthetic and as an antidepressant for treatment of depression. It is sold under the brand names Spravato, Ketanest, among others. Esketamine is the active enantiomer of ketamine in terms of NMDA receptor antagonism and is more potent than racemic ketamine.

Major depressive disorder, often simply referred to as depression, is a mental disorder characterized by prolonged unhappiness or irritability. It is accompanied by a constellation of somatic and cognitive signs and symptoms such as fatigue, apathy, sleep problems, loss of appetite, loss of engagement, low self-regard/worthlessness, difficulty concentrating or indecisiveness, or recurrent thoughts of death or suicide.

Eric J. Nestler is the Nash Family Professor of Neuroscience, Director of the Friedman Brain Institute, and Dean for Academic Affairs at the Icahn School of Medicine at Mount Sinai and Chief Scientific Officer of the Mount Sinai Health System. His research is focused on a molecular approach to drug addiction and depression.

Arketamine (developmental code names PCN-101, HR-071603), also known as (R)-ketamine or (R)-(−)-ketamine, is the (R)-(−) enantiomer of ketamine. Similarly to racemic ketamine and esketamine, the S(+) enantiomer of ketamine, arketamine is biologically active; however, it is less potent as an NMDA receptor antagonist and anesthetic and thus has never been approved or marketed for clinical use as an enantiopure drug. Arketamine is currently in clinical development as a novel antidepressant.

Hydroxynorketamine (HNK), or 6-hydroxynorketamine, is a minor metabolite of the anesthetic, dissociative, and antidepressant drug ketamine. It is formed by hydroxylation of the intermediate norketamine, another metabolite of ketamine. As of late 2019, (2R,6R)-HNK is in clinical trials for the treatment of depression.
Joseph Zohar is the director of Psychiatry and the Anxiety and Obsessive Compulsive Clinic at the Sheba Medical Center in Tel HaShomer and professor of psychiatry at Tel Aviv University, Israel. He is the founder of the World Council on Anxiety as well as the Israeli Consortium on PTSD. He currently leads the chief installation of the Israeli Defense Force for the treatment of PTSD. He is a member of the executive committee of the European College of Neuropsychopharmacology, of which he is a former president, and chairman of the Expert Platform on Mental Health.
Lisa M. Monteggia is an American neuroscientist who is a Professor in the Department of Pharmacology, Psychiatry & Psychology as well as the Barlow Family Director of the Vanderbilt Brain Institute at Vanderbilt University in Nashville, Tennessee. Monteggia probes the molecular mechanisms underlying psychiatric disorders and has made critical discoveries about the role of the neurotrophins in antidepressant efficacy, the antidepressant mechanisms of Ketamine, as well as the epigenetic regulation of synaptic transmission by MeCP2.

Carolyn I. Rodriguez is a Puerto Rican psychiatrist, neuroscientist, and clinical researcher developing treatments for obsessive compulsive disorder as well as mapping circuit dysfunction in the human brain. Rodriguez holds appointments in both clinical and academic departments at Stanford University. Rodriguez is a Clinical Lab Director at the Stanford Center for Cognitive and Neurobiological Imaging, an associate professor and Associate Chair of Psychiatry and Behavioral Sciences, and a Director of several specialized translational research programs.
Gabriella Gobbi is an Italo-Canadian psychiatrist and neuroscientist whose research explores novel treatments for mental health disorders. Gobbi is a professor at McGill University's Department of Psychiatry and a Canada Research Chair in Therapeutics for Mental Health.
Ketamine-assisted psychotherapy(KAP) is the use of prescribed doses of ketamine, the drug, as an adjunct to psychotherapy sessions. KAP shows significant potential in treating mental disorders such as treatment-resistant depression (TRD), anxiety, obsessive–compulsive disorders (OCD), post-traumatic stress disorders (PTSD), and other conditions. It can also be used for those experiencing substance abuse and physical pain. While it is primarily used as a veterinary anaesthetic, ketamine has also been found to have rapid analgesic and hallucinogenic effects, which has sparked interest in its use as an antidepressant. Despite initial trials of its use in the treatment of mental disorders focussing primarily on its antidepressant effects, newer studies are attempting to harness its psychedelic effects to bring about altered states of consciousness, which will augment the adjunct psychotherapy. Ketamine's neuroplasticity-promoting effects strengthen the cognitive restructuring that takes place through traditional psychotherapy, thereby leading to long-lasting behavioural change. KAP offers promising directions for research on new antidepressant alternatives, but is still not sufficiently defined or evaluated as a treatment combination.










