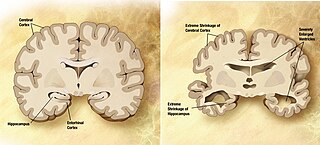
A neurodegenerative disease is caused by the progressive loss of structure or function of neurons, in the process known as neurodegeneration. Such neuronal damage may ultimately involve cell death. Neurodegenerative diseases include amyotrophic lateral sclerosis, multiple sclerosis, Parkinson's disease, Alzheimer's disease, Huntington's disease, multiple system atrophy, and prion diseases. Neurodegeneration can be found in the brain at many different levels of neuronal circuitry, ranging from molecular to systemic. Because there is no known way to reverse the progressive degeneration of neurons, these diseases are considered to be incurable; however research has shown that the two major contributing factors to neurodegeneration are oxidative stress and inflammation. Biomedical research has revealed many similarities between these diseases at the subcellular level, including atypical protein assemblies and induced cell death. These similarities suggest that therapeutic advances against one neurodegenerative disease might ameliorate other diseases as well.

In medicine, proteinopathy, or proteopathy, protein conformational disorder, or protein misfolding disease, is a class of diseases in which certain proteins become structurally abnormal, and thereby disrupt the function of cells, tissues and organs of the body. Often the proteins fail to fold into their normal configuration; in this misfolded state, the proteins can become toxic in some way or they can lose their normal function. The proteinopathies include such diseases as Creutzfeldt–Jakob disease and other prion diseases, Alzheimer's disease, Parkinson's disease, amyloidosis, multiple system atrophy, and a wide range of other disorders. The term proteopathy was first proposed in 2000 by Lary Walker and Harry LeVine.

Shinya Yamanaka is a Japanese stem cell researcher and a Nobel Prize laureate. He is the former director of Center for iPS Cell Research and Application and a professor at the Institute for Frontier Medical Sciences at Kyoto University; as a senior investigator at the UCSF-affiliated Gladstone Institutes in San Francisco, California; and as a professor of anatomy at University of California, San Francisco (UCSF). Yamanaka is also a past president of the International Society for Stem Cell Research (ISSCR).

Transmembrane protein 106B is a protein that is encoded by the TMEM106B gene. It is found primarily within neurons and oligodendrocytes in the central nervous system with its subcellular location being in lysosomal membranes. TMEM106B helps facilitate important functions for maintaining a healthy lysosome, and therefore certain mutations and polymorphisms can lead to issues with proper lysosomal function. Lysosomes are in charge of clearing out mis-folded proteins and other debris, and thus, play an important role in neurodegenerative diseases that are driven by the accumulation of various mis-folded proteins and aggregates. Due to its impact on lysosomal function, TMEM106B has been investigated and found to be associated to multiple neurodegenerative diseases.
John Quinn Trojanowski was an American academic research neuroscientist specializing in neurodegeneration. He and his partner, Virginia Man-Yee Lee, MBA, Ph.D., are noted for identifying the roles of three proteins in neurodegenerative diseases: tau in Alzheimer's disease, alpha-synuclein in Parkinson's disease, and TDP-43 in Amyotrophic Lateral Sclerosis (ALS) and frontotemporal degeneration.
Samuel E. Gandy, M.D., Ph.D. is a neurologist, cell biologist, Alzheimer's disease (AD) researcher and expert in the metabolism of the sticky substance called amyloid that clogs the brain in patients with Alzheimer's. His team discovered the first drugs that could lower the formation of amyloid.

Anne Buckingham Young is an American physician and neuroscientist who has made major contributions to the study of neurodegenerative diseases, with a focus on movement disorders like Huntington's disease and Parkinson's disease. Young completed her undergraduate studies at Vassar College and earned a dual MD/PhD from Johns Hopkins Medical School. She has held faculty positions at University of Michigan and Harvard University. She became the first female chief of service at Massachusetts General Hospital when she was appointed Chief of Neurology in 1991. She retired from this role and from clinical service in 2012. She is a member of many academic societies and has won numerous awards. Young is also the only person to have been president of both the international Society for Neuroscience and the American Neurological Association.

The Krembil Research Institute, formerly known as the Toronto Western Research Institute, is an academic medical research institute in Toronto. It is one of the largest research institutes in Canada focusing on human neurological disease.

Virginia Man-Yee Lee is a Chinese-born American biochemist and neuroscientist who specializes in the research of Alzheimer's disease. She is the current John H. Ware 3rd Endowed Professor in Alzheimer's Research at the Department of Pathology and Laboratory Medicine, and the director of the Center for Neurodegenerative Disease Research and co-director of the Marian S. Ware Alzheimer Drug Discovery Program at the Perelman School of Medicine, University of Pennsylvania. She received the 2020 Breakthrough Prize in Life Sciences.

Nevan J. Krogan is a Canadian molecular and systems biologist. He is a professor and the Director of the Quantitative Biosciences Institute (QBI) at the University of California San Francisco (UCSF), as well as a senior investigator at the J. David Gladstone Institutes.
Benjamin Wolozin is an American pharmacologist and neurologist currently at Boston University School of Medicine and an Elected Fellow of the American Association for the Advancement of Science. Benjamin Wolozin, M.D., Ph.D. received his B.A. from Wesleyan University and his M.D., Ph.D. from the Albert Einstein College of Medicine. He is currently a professor of Pharmacology, Neurology and the Program in Neuroscience at Boston University School of Medicine. He is also co-founder and Chief Scientific Officer (CSO) of Aquinnah Pharmaceuticals Inc., a biotechnology company developing novel therapeutics to treat Alzheimer's disease and Amyotrophic Lateral Sclerosis.

Rahul Desikan was an Indian-American neuroscientist and neuroradiologist. He was an Assistant Professor of Radiology & Biomedical Imaging, Neurology and Pediatrics at the University of California, San Francisco, and co-director of Laboratory for Precision Neuroimaging. Desikan's achievements became publicly known in a Washington Post article detailing his lifelong commitment to preventing and treating Alzheimer's disease and his continuing work as a scientist living with Amyotrophic lateral sclerosis (ALS). Desikan was vocal about the need for increased awareness and research funding for ALS, and voiced his unique perspective as both ALS researcher and ALS patient in op-ed articles appearing in a regular column in the Washington Post as well as in the San Francisco Chronicle and Scientific American.
Thea D. Tlsty is an American pathologist and professor of pathology at the University of California, San Francisco (UCSF). She is known for her research in cancer biology and her involvement in the discovery of cells that may be at the origin of metaplastic cancer, an invasive form of breast cancer.
Çağhan Kızıl is a Turkish/German neuroscientist and geneticist, and Associate Professor of Neurological Sciences at the Taub Institute for Research on Alzheimer's Disease and the Aging Brain at the Columbia University Vagelos College of Physicians and Surgeons Columbia University Irving Medical Center.

Nancy M. Bonini is an American neuroscientist and geneticist, best known for pioneering the use of Drosophila as a model organism to study neurodegeneration of the human brain. Using the Drosophila model approach, Bonini's laboratory has identified genes and pathways that are important in the development and progression of neurodegenerative diseases such as Amyotrophic lateral sclerosis, Alzheimer's disease, and Parkinson's disease, as well as aging, neural injury and regeneration, and response to environmental toxins.
Dena Dubal is the David A. Coulter Endowed Chair in Ageing and Neurodegenerative Disease at University of California, San Francisco. Dubal has demonstrated that the hormone Klotho can enhance cognition and protect the brain from neurodegenerative decline.

Phenserine is a synthetic drug which has been investigated as a medication to treat Alzheimer's disease (AD), as the drug exhibits neuroprotective and neurotrophic effects.

Katerina Akassoglou is a neuroimmunologist who is a Senior Investigator and Director of In Vivo Imaging Research at the Gladstone Institutes. Akassoglou holds faculty positions as a Professor of Neurology at the University of California, San Francisco. Akassoglou has pioneered investigations of blood-brain barrier integrity and development of neurological diseases. She found that compromised blood-brain barrier integrity leads to fibrinogen leakage into the brain inducing neurodegeneration. Akassoglou is internationally recognized for her scientific discoveries.
David Rowitch, FMedSci, FRS is an American physician-scientist known for his contributions to developmental glial biology and treatment of white matter diseases. He heads the Department of Paediatrics at the University of Cambridge and is an adjunct professor of pediatrics at the University of California San Francisco (UCSF).
Li Gan is a neuroscientist and professor at Weill Cornell Medical College. She is known for her discovery of pathogenic tau protein acetylation in tauopathies and mechanisms of microglia dysfunction in neurodegeneration.













