
Avian influenza, known informally as avian flu, is a bird flu caused by the influenza A virus, which can infect people. It is similar to other types of animal flu in that it is caused by a virus strain that has adapted to a specific host. The type with the greatest risk is highly pathogenic avian influenza (HPAI).

Influenza A virus subtype H5N1 (A/H5N1) is a subtype of the influenza A virus which can cause illness in humans and many other species. A bird-adapted strain of H5N1, called HPAI A(H5N1) for highly pathogenic avian influenza virus of type A of subtype H5N1, is the highly pathogenic causative agent of H5N1 flu, commonly known as avian influenza. It is enzootic in many bird populations, especially in Southeast Asia. One strain of HPAI A(H5N1) is spreading globally after first appearing in Asia. It is epizootic and panzootic, killing tens of millions of birds and spurring the culling of hundreds of millions of others to stem its spread. Many references to "bird flu" and H5N1 in the popular media refer to this strain.
Singapore has taken a series of measures against avian influenza and the potential threat of a pandemic.

Bernard Matthews Foods Limited is a British farming and food products business with its headquarters in Great Witchingham, Norfolk, England, which specialises in turkey products.

The global spread of H5N1 influenza in birds is considered a significant pandemic threat. While other H5N1 influenza strains are known, they are significantly different on a genetic level from a recent, highly pathogenic, emergent strain of H5N1, which was able to achieve hitherto unprecedented global spread in 2008. The H5N1 strain is a fast-mutating, highly pathogenic avian influenza virus (HPAI) found in multiple bird species. It is both epizootic and panzootic. Unless otherwise indicated, "H5N1" in this timeline refers to the recent highly pathogenic strain of H5N1.

Transmission and infection of H5N1 from infected avian sources to humans has been a concern since the first documented case of human infection in 1997, due to the global spread of H5N1 that constitutes a pandemic threat.

H5 N2 is a subtype of the species Influenzavirus A. The subtype infects a wide variety of birds, including chickens, ducks, turkeys, falcons, and ostriches. Affected birds usually do not appear ill, and the disease is often mild as avian influenza viral subtypes go. Some variants of the subtype are much more pathogenic than others, and outbreaks of "high-path" H5N2 result in the culling of thousands of birds in poultry farms from time to time. It appears that people who work with birds can be infected by the virus, but suffer hardly any noticeable health effects. Even people exposed to the highly pathogenic H5N2 variety that killed ostrich chicks in South Africa only seem to have developed conjunctivitis, or a perhaps a mild respiratory illness. There is no evidence of human-to-human spread of H5N2. On November 12, 2005 it was reported that a falcon was found to have H5N2.

Influenza A virus subtype H7N7 (A/H7N7) is a subtype of Influenza A virus, a genus of Orthomyxovirus, the viruses responsible for influenza. Highly pathogenic strains (HPAI) and low pathogenic strains (LPAI) exist. H7N7 can infect humans, birds, pigs, seals, and horses in the wild; and has infected mice in laboratory studies. This unusual zoonotic potential represents a pandemic threat.

Influenza A virus subtype H7N2 (A/H7N2) is a subtype of the species Influenza A virus. This subtype is one of several sometimes called bird flu virus. H7N2 is considered a low pathogenicity avian influenza (LPAI) virus. With this in mind, H5 & H7 influenza viruses can re-assort into the Highly Pathogenic variant if conditions are favorable.

Influenza A virus subtype H7N3 (A/H7N3) is a subtype of the species Influenza A virus.

H5N8 is a subtype of the influenza A virus and is highly lethal to wild birds and poultry. H5N8 is typically not associated with humans. However, seven people in Russia were found to be infected in 2021, becoming the first documented human cases.

The social impact of H5N1 is the effect or influence of H5N1 in human society; especially the financial, political, social, and personal responses to both actual and predicted deaths in birds, humans, and other animals. Billions of dollars are being raised and spent to research H5N1 and prepare for a potential avian influenza pandemic. Over ten billion dollars have been lost and over two hundred million birds have been killed to try to contain H5N1. People have reacted by buying less chicken causing poultry sales and prices to fall. Many individuals have stockpiled supplies for a possible flu pandemic.

The global spread of H5N1 in birds is considered a significant pandemic threat.

The global spread of H5N1 in birds is considered a significant pandemic threat.

The 2008 bird flu outbreak in West Bengal is an occurrence of avian influenza in West Bengal, India that began on January 16, 2008. The infection was caused by the H5N1 subtype of the Influenza A virus and occurred in at least thirteen districts, including Birbhum, Nadia, Murshidabad, Burdwan, Hooghly, Cooch Behar, Malda, Bankura, Purulia, Howrah, West Midnapore, South 24 Parganas and South Dinajpur and several new inclusion are reported daily. A range of precautions has been instituted including a large cull of chickens, eggs, and poultry birds, the imposition of segregation zones, and a disinfection programme for the plant. The government had put a blanket ban on the movement of poultry birds from West Bengal.

The global spread of H5N1 in birds is considered a significant pandemic threat.

H5N6 is a subtype of the species Influenza A virus. Infected birds shed the virus in their saliva, mucous, and feces. The virus was first detected in poultry in 2013, since then spreading among wild bird populations and poultry around the world. Humans can be infected through unprotected contact with infected birds or contaminated surfaces. The virus transmits by getting into a person's eyes, nose, mouth, and through inhalation. Human infections are rare. Since 2014, at least 65 cases have occurred in humans. 29 people have died. A spike in human cases was reported in 2021. There have been no confirmed cases of human-to-human transmission. Some infections have been identified where no direct contact with infected birds or contaminated surfaces has been known to had occurred. Only one infected woman has said that she never came into any contact with poultry.

In 2015, an outbreak of avian influenza subtype H5N2 was identified in a series of chicken and turkey farming operations in the Midwestern United States. By May 30, more than 43 million birds in 15 states had been destroyed as a result of the outbreak, including nearly 30 million in Iowa alone, the nation's largest egg producer. In the Midwestern U.S., the average price of eggs had increased 120% between April 22 and May 30. The effects however were seen nationwide, with prices in California up 71% in the same timeframe.
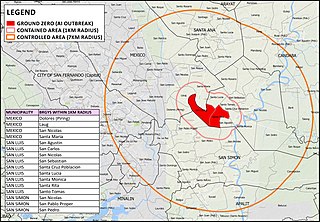
From April to September 2017 in the Philippines, an outbreak of H5N6 avian influenza or bird flu affected poultry in at least three towns in Central Luzon; San Luis in Pampanga and Jaen and San Isidro in Nueva Ecija.

In the early 2020s, an ongoing outbreak of avian influenza subtype H5N8 has been occurring at poultry farms and among wild bird populations in several countries and continents, leading to the subsequent cullings of millions of birds to prevent a pandemic similar to that of the H5N1 outbreak in 2008. The first case of human transmission of avian flu, also known as bird flu, was reported by Russian authorities in February 2021, as several poultry farm workers tested positive for the virus.







