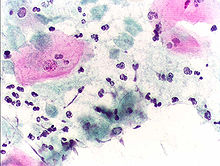
Bacterial vaginosis (BV) is an infection of the vagina caused by excessive growth of bacteria. Common symptoms include increased vaginal discharge that often smells like fish. The discharge is usually white or gray in color. Burning with urination may occur. Itching is uncommon. Occasionally, there may be no symptoms. Having BV approximately doubles the risk of infection by a number of sexually transmitted infections, including HIV/AIDS. It also increases the risk of early delivery among pregnant women.

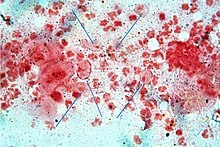
Trichomoniasis (trich) is an infectious disease caused by the parasite Trichomonas vaginalis. About 70% of affected people do not have symptoms when infected. When symptoms occur, they typically begin 5 to 28 days after exposure. Symptoms can include itching in the genital area, a bad smelling thin vaginal discharge, burning with urination, and pain with sex. Having trichomoniasis increases the risk of getting HIV/AIDS. It may also cause complications during pregnancy.
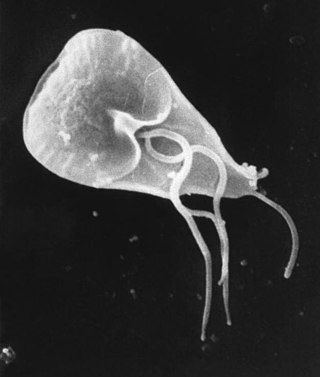
Giardia is a genus of anaerobic flagellated protozoan parasites of the phylum Metamonada that colonise and reproduce in the small intestines of several vertebrates, causing the disease giardiasis. Their life cycle alternates between a swimming trophozoite and an infective, resistant cyst. Giardia were first described by the Dutch microscopist Antonie van Leeuwenhoek in 1681. The genus is named after French zoologist Alfred Mathieu Giard.

Giardia duodenalis, also known as Giardia intestinalis and Giardia lamblia, is a flagellated parasitic protozoan microorganism of the genus Giardia that colonizes the small intestine, causing a diarrheal condition known as giardiasis. The parasite attaches to the intestinal epithelium by an adhesive disc or sucker, and reproduces via binary fission. Giardiasis does not spread to other parts of the gastrointestinal tract, but remains confined to the lumen of the small intestine. The microorganism has an outer membrane that makes it possible to survive even when outside of its host, and which can render it tolerant to certain disinfectants. Giardia trophozoites are anaerobic, and absorb their nutrients from the intestinal lumen. If the organism is stained, its characteristic pattern resembles the familiar "smiley face" symbol.
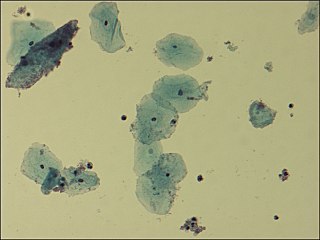
Gardnerella vaginalis is a species of Gram-variable-staining facultative anaerobic bacteria. The organisms are small non-spore-forming, nonmotile coccobacilli.

Metronidazole, sold under the brand name Flagyl among others, is an antibiotic and antiprotozoal medication. It is used either alone or with other antibiotics to treat pelvic inflammatory disease, endocarditis, and bacterial vaginosis. It is effective for dracunculiasis, giardiasis, trichomoniasis, and amebiasis. It is an option for a first episode of mild-to-moderate Clostridioides difficile colitis if vancomycin or fidaxomicin is unavailable. Metronidazole is available orally, as a cream or gel, and by slow intravenous infusion.
Vaginitis, also known as vulvovaginitis, is inflammation of the vagina and vulva. Symptoms may include itching, burning, pain, discharge, and a bad smell. Certain types of vaginitis may result in complications during pregnancy.

Acanthamoeba is a genus of amoebae that are commonly recovered from soil, fresh water, and other habitats. The genus Acanthamoeba has two stages in its life cycle, the metabolically active trophozoite stage and a dormant, stress-resistant cyst stage. In nature, Acanthamoeba species are generally free-living bacterivores. However, they are also opportunistic pathogens able to cause serious and sometimes fatal infections in humans and other animals.

Giardiasis is a parasitic disease caused by Giardia duodenalis. Infected individuals who experience symptoms may have diarrhoea, abdominal pain, and weight loss. Less common symptoms include vomiting and blood in the stool. Symptoms usually begin one to three weeks after exposure and, without treatment, may last two to six weeks or longer.

The parabasalids are a group of flagellated protists within the supergroup Excavata. Most of these eukaryotic organisms form a symbiotic relationship in animals. These include a variety of forms found in the intestines of termites and cockroaches, many of which have symbiotic bacteria that help them digest cellulose in woody plants. Other species within this supergroup are known parasites, and include human pathogens.

Trichomonas is a genus of anaerobic excavate parasites of vertebrates. It was first discovered by Alfred François Donné in 1836 when he found these parasites in the pus of a patient suffering from vaginitis, an inflammation of the vagina. Donné named the genus from its morphological characteristics. The prefix tricho- originates from the Ancient Greek word θρίξ (thrix) meaning hair, describing Trichomonas’s flagella. The suffix -monas, describes its similarity to unicellular organisms from the genus Monas.

Tritrichomonas foetus is a species of single-celled flagellated parasites that is known to be a pathogen of the bovine reproductive tract as well as the intestinal tract of cats. In cattle, the organism is transmitted to the female vagina and uterus from the foreskin of the bull where the parasite is known to reside. It causes infertility, and, at times, has caused spontaneous abortions in the first trimester. In the last ten years, there have been reports of Tritrichomonas foetus in the feces of young cats that have diarrhea and live in households with multiple cats. Tritrichomonas foetus looks similarly to Giardia and is often misdiagnosed for it when viewed under a microscope.

Protozoan infections are parasitic diseases caused by organisms formerly classified in the kingdom Protozoa. These organisms are now classified in the supergroups Excavata, Amoebozoa, Harosa, and Archaeplastida. They are usually contracted by either an insect vector or by contact with an infected substance or surface.

A sexually transmitted infection (STI), also referred to as a sexually transmitted disease (STD) and the older term venereal disease (VD), is an infection that is spread by sexual activity, especially vaginal intercourse, anal sex, oral sex, or sometimes manual sex. STIs often do not initially cause symptoms, which results in a risk of passing the infection on to others. Symptoms and signs of STIs may include vaginal discharge, penile discharge, ulcers on or around the genitals, and pelvic pain. Some STIs can cause infertility.
Female genital disease is a disorder of the structure or function of the female reproductive system that has a known cause and a distinctive group of symptoms, signs, or anatomical changes. The female reproductive system consists of the ovaries, fallopian tubes, uterus, vagina, and vulva. Female genital diseases can be classified by affected location or by type of disease, such as malformation, inflammation, or infection.

Trichomonas gallinae is a cosmopolitan parasite of birds including finches, pigeons, doves, turkeys, chickens, parrots, raptors. The condition in birds of prey is called frounce. It is believed to be an ancient pathogen causing frounce-like symptoms in theropod dinosaurs. The same condition in pigeons is commonly called canker.
In biology, a pathogen, in the oldest and broadest sense, is any organism or agent that can produce disease. A pathogen may also be referred to as an infectious agent, or simply a germ.

Trichomonas tenax, or oral trichomonas, is a species of Trichomonas commonly found in the oral cavity of humans. Routine hygiene is generally not sufficient to eliminate the parasite, hence its Latin name, meaning "tenacious". The parasite is frequently encountered in periodontal infections, affecting more than 50% of the population in some areas, but it is usually considered insignificant. T. tenax is generally not found on the gums of healthy patients. It is known to play a pathogenic role in necrotizing ulcerative gingivitis and necrotizing ulcerative periodontitis, worsening preexisting periodontal disease. This parasite is also implicated in some chronic lung diseases; in such cases, removal of the parasite is sufficient to allow recovery.
Patricia Jean Johnson is a Professor of Microbiology at University of California, Los Angeles (UCLA). She works on the parasite Trichomonas vaginalis, which is responsible for the most prevalent sexually transmitted infections in the United States, Trichomoniasis. She was elected a member of the National Academy of Sciences (NAS) in 2019.

Lactobacillus vaccines are used in the therapy and prophylaxis of non-specific bacterial vaginitis and trichomoniasis. The vaccines consist of specific inactivated strains of Lactobacilli, called "aberrant" strains in the relevant literature dating from the 1980s. These strains were isolated from the vaginal secretions of patients with acute colpitis. The lactobacilli in question are polymorphic, often shortened or coccoid in shape and do not produce an acidic, anti-pathogenic vaginal environment. A colonization with aberrant lactobacilli has been associated with an increased susceptibility to vaginal infections and a high rate of relapse following antimicrobial treatment. Intramuscular administration of inactivated aberrant lactobacilli provokes a humoral immune response. The production of specific antibodies both in serum and in the vaginal secretion has been demonstrated. As a result of the immune stimulation, the abnormal lactobacilli are inhibited, the population of normal, rod-shaped lactobacilli can grow and exert its defense functions against pathogenic microorganisms.