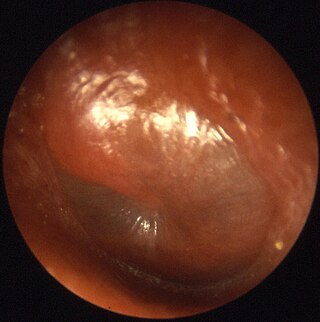
Otitis media is a group of inflammatory diseases of the middle ear. One of the two main types is acute otitis media (AOM), an infection of rapid onset that usually presents with ear pain. In young children this may result in pulling at the ear, increased crying, and poor sleep. Decreased eating and a fever may also be present. The other main type is otitis media with effusion (OME), typically not associated with symptoms, although occasionally a feeling of fullness is described; it is defined as the presence of non-infectious fluid in the middle ear which may persist for weeks or months often after an episode of acute otitis media. Chronic suppurative otitis media (CSOM) is middle ear inflammation that results in a perforated tympanic membrane with discharge from the ear for more than six weeks. It may be a complication of acute otitis media. Pain is rarely present. All three types of otitis media may be associated with hearing loss. If children with hearing loss due to OME do not learn sign language, it may affect their ability to learn.

Earwax, also known by the medical term cerumen, is a brown, orange, red, yellowish or gray waxy substance secreted in the ear canal of humans and other mammals. It protects the skin of the human ear canal, assists in cleaning and lubrication, and provides protection against bacteria, fungi, and water.
Benzocaine, sold under the brand name Orajel amongst others, is an ester local anesthetic commonly used as a topical pain reliever or in cough drops. It is the active ingredient in many over-the-counter anesthetic ointments such as products for oral ulcers. It is also combined with antipyrine to form A/B otic drops to relieve ear pain and remove earwax. In the US, products containing benzocaine for oral application are contraindicated in children younger than two years old. In the European Union, the contraindication applies to children under 12 years of age.

An earplug is a device that is inserted in the ear canal to protect the user's ears from loud noises, intrusion of water, foreign bodies, dust or excessive wind. Since they reduce the sound volume, earplugs are often used to help prevent hearing loss and tinnitus.

Conductive hearing loss (CHL) occurs when there is a problem transferring sound waves anywhere along the pathway through the outer ear, tympanic membrane (eardrum), or middle ear (ossicles). If a conductive hearing loss occurs in conjunction with a sensorineural hearing loss, it is referred to as a mixed hearing loss. Depending upon the severity and nature of the conductive loss, this type of hearing impairment can often be treated with surgical intervention or pharmaceuticals to partially or, in some cases, fully restore hearing acuity to within normal range. However, cases of permanent or chronic conductive hearing loss may require other treatment modalities such as hearing aid devices to improve detection of sound and speech perception.

The ear canal is a pathway running from the outer ear to the middle ear. The adult human ear canal extends from the pinna to the eardrum and is about 2.5 centimetres (1 in) in length and 0.7 centimetres (0.3 in) in diameter.

Ear pain, also known as earache or otalgia, is pain in the ear. Primary ear pain is pain that originates from the ear. Secondary ear pain is a type of referred pain, meaning that the source of the pain differs from the location where the pain is felt.

Tympanostomy tube, also known as a grommet or myringotomy tube, is a small tube inserted into the eardrum in order to keep the middle ear aerated for a prolonged period of time, and to prevent the accumulation of fluid in the middle ear. The operation to insert the tube involves a myringotomy and is performed under local or general anesthesia. The tube itself is made in a variety of designs. The most commonly used type is shaped like a grommet. When it is necessary to keep the middle ear ventilated for a very long period, a "T"-shaped tube may be used, as these "T-tubes" can stay in place for 2–4 years. Materials used to construct the tube are most often plastics such as silicone or Teflon. Stainless steel tubes exist, but are no longer in frequent use.

Otitis is a general term for inflammation or infection, inner ear infection, middle ear infection of the ear, in both humans and other animals. When infection is present, it may be viral or bacterial. When inflammation is present due to fluid build up in the middle ear and infection is not present it is considered Otitis media with effusion. It is subdivided into the following:

Ear mites are mites that live in the ears of animals and humans. The most commonly seen species in veterinary medicine is Otodectes cynotis. This species, despite its name, is also responsible for 90% of ear mite infections in felines.

An otoscope or auriscope is a medical device which is used to look into the ears. Health care providers use otoscopes to screen for illness during regular check-ups and also to investigate ear symptoms. An otoscope potentially gives a view of the ear canal and tympanic membrane or eardrum. Because the eardrum is the border separating the external ear canal from the middle ear, its characteristics can be indicative of various diseases of the middle ear space. The presence of earwax (cerumen), shed skin, pus, canal skin edema, foreign body, and various ear diseases can obscure any view of the eardrum and thus severely compromise the value of otoscopy done with a common otoscope, but confirm the presence of obstructing symptoms.

Ciprofloxacin/dexamethasone (Ciprodex) is an antibiotic/steroid combination medication. It contains the synthetic broad-spectrum antibacterial agent, ciprofloxacin hydrochloride (0.3%), combined with the anti-inflammatory corticosteroid, dexamethasone (0.1%), in a sterile, preserved suspension for otic use.
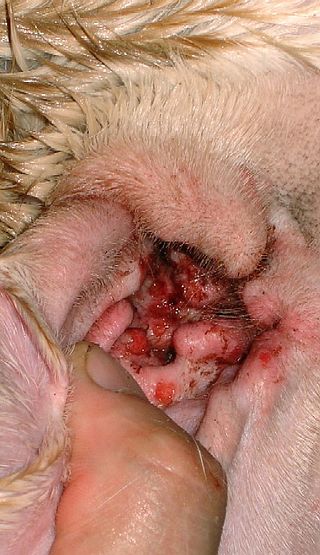
Otitis externa is an inflammation of the outer ear and ear canal. Animals are commonly prone to ear infection, and this is one of the most common manifestations of allergy in dogs. In dogs, those breeds with floppy ears are more prone, since air flow is limited and a warm, moist environment built up, which is conducive to infection. The external ear in animals is longer and deeper than in humans, which makes it easier for infection or wax to build up or be hard to remove. Complete ear canal inspection requires the use of an otoscope by a veterinarian.
Otomycosis is a fungal ear infection, a superficial mycotic infection of the outer ear canal. It is more common in tropical countries. The infection may be either subacute or acute and is characterized by malodorous discharge, inflammation, pruritus, scaling, and severe discomfort. The mycosis results in inflammation, superficial epithelial exfoliation, masses of debris containing hyphae, suppuration, and pain.
Neomycin/polymyxin B/hydrocortisone, sold under the brand Otosporin among others, is a medication used to treat otitis externa and certain eye disorders. It consists of the antibiotics neomycin and polymyxin B, and the steroid hydrocortisone. It is used as an ear drop or eye drop.
Ear instillation is the process of introducing otic medication or other liquids into the ear canal. Proper care is needed in delivering such liquids.

Otitis externa, also called swimmer's ear, is inflammation of the ear canal. It often presents with ear pain, swelling of the ear canal, and occasionally decreased hearing. Typically there is pain with movement of the outer ear. A high fever is typically not present except in severe cases.

Finafloxacin (Xtoro) is a fluoroquinolone antibiotic. In the United States, it is approved by the Food and Drug Administration to treat acute otitis externa caused by the bacteria Pseudomonas aeruginosa and Staphylococcus aureus.

A cerumenolytic is an ear wax (cerumen) softening agent. Common cerumenolytics such as hydrogen peroxide and hydrogen peroxide - urea are topical preparations used to facilitate the removal of ear wax. Their side effects tend to be mild, including ear discomfort, transient loss of hearing, dizziness, and local irritation.
Middle ear barotrauma (MEBT), also known to underwater divers as ear squeeze and reverse ear squeeze, is an injury caused by a difference in pressure between the external ear canal and the middle ear. It is common in underwater divers and usually occurs when the diver does not equalise sufficiently during descent or, less commonly, on ascent. Failure to equalise may be due to inexperience or eustachian tube dysfunction, which can have many possible causes. Unequalised ambient pressure increase during descent causes a pressure imbalance between the middle ear air space and the external auiditory canal over the eardrum, referred to by divers as ear squeeze, causing inward stretching, serous effusion and haemorrhage, and eventual rupture. During ascent internal over-pressure is normally passively released through the eustachian tube, but if this does not happen the volume expansion of middle ear gas will cause outward bulging, stretching and eventual rupture of the eardrum known to divers as reverse ear squeeze. This damage causes local pain and hearing loss. Tympanic rupture during a dive can allow water into the middle ear, which can cause severe vertigo from caloric stimulation. This may cause nausea and vomiting underwater, which has a high risk of aspiration of vomit or water, with possible fatal consequences.